Parasomnias
Parasomnias Diagnosis & Treatment at Mir Neurology
What are Parasomnias?
Parasomnias are a group of sleep disorders that involve abnormal behaviors, movements, or experiences that occur during sleep. These disorders can disrupt both the individual experiencing them and those around them. Unlike typical sleep-related activities such as snoring or talking in your sleep, parasomnias involve unusual, often disturbing actions during sleep stages, such as sleepwalking, nightmares, night terrors, or REM sleep behavior disorder.
At Mir Neurology, we are committed to diagnosing and treating parasomnias, helping patients regain control over their sleep, and improving their overall well-being.
Types of Parasomnias
Parasomnias can occur during different stages of sleep, including non-REM (Rapid Eye Movement) and REM sleep. The most common parasomnias include:
1. Sleepwalking (Somnambulism):
Sleepwalking typically occurs during deep non-REM sleep (stage 3 or 4) and involves walking or performing other complex behaviors while still asleep.
Individuals who sleepwalk may appear awake but are not conscious of their actions and usually have little to no memory of the event upon waking.
Sleepwalking can involve walking around the house, eating, or even leaving the house. In some cases, it may be dangerous.


2. Nightmares:
Nightmares are vivid, disturbing dreams that usually occur during REM sleep and often lead to waking up feeling anxious or frightened.
While everyone experiences nightmares occasionally, frequent nightmares may indicate underlying issues such as anxiety, stress, or other mental health disorders.
3. Night Terrors (Sleep Terrors):
Night terrors occur during non-REM sleep, usually in the first few hours of the night.
Individuals experiencing night terrors may suddenly sit up in bed, scream, or act as if they are in a state of intense fear. They may have rapid breathing, increased heart rate, and appear to be in distress.
Unlike nightmares, people experiencing night terrors typically do not remember the event upon waking.
4. REM Sleep Behavior Disorder (RBD):
REM Sleep Behavior Disorder occurs when the normal muscle paralysis during REM sleep is absent, leading to the acting out of dreams.
Individuals with RBD may physically move, talk, or even engage in violent behaviors while still asleep, such as kicking, punching, or jumping out of bed.
These behaviors can be potentially harmful to the person or their sleep partner and often involve vivid, intense dreams that the individual recalls upon waking.
5. Sleep Eating Disorder:
People with sleep eating disorders eat while they are asleep, often consuming unusual or non-nutritious foods.
Like sleepwalking, individuals are unaware of their actions and may have little to no memory of eating once they wake up.


6. Sleep Paralysis:
Sleep paralysis occurs when a person wakes up during REM sleep but is temporarily unable to move or speak. This experience is often accompanied by vivid hallucinations or a feeling of pressure on the chest.
Though frightening, sleep paralysis is generally harmless and can occur in people with no other sleep disorders.
7. Teeth Grinding (Bruxism):
Bruxism involves grinding or clenching the teeth, usually during deep sleep.
It can lead to jaw pain, tooth wear, and headaches and may affect the quality of sleep for both the individual and their partner.
The symptoms of parasomnias depend on the type of disorder but can include:
Symptoms vary depending on the specific disorder and severity.
Movement or behavior during sleep (e.g., walking, kicking, or punching).
Loud noises, such as screaming, shouting, or talking.
Sleep disruptions, include waking up suddenly, experiencing confusion, or being unable to fall back asleep.
Memory gaps regarding what occurred during sleep.
Injury due to unsafe movements, such as falling or bumping into objects.
Daytime fatigue caused by disrupted sleep.
If you or someone you know is experiencing any of these symptoms, it may be time to seek medical advice to identify the cause and receive proper treatment.
Causes of Parasomnias
Parasomnias often result from a combination of biological, psychological, and environmental factors.
1. Sleep Deprivation:
Emotional stress, anxiety, or unresolved trauma can increase the frequency of parasomnias. Conditions like PTSD (Post-Traumatic Stress Disorder) are particularly associated with night terrors and nightmares. Insufficient sleep disrupts normal sleep architecture and increases abnormal behaviors.


2. Stress and Anxiety:
Stress and anxiety keep your mind active during sleep instead of letting your body fully rest. This ongoing mental tension disrupts normal sleep cycles. As a result, unusual sleep behaviors such as sleepwalking, night terrors, or talking during sleep can occur.
3. Sleep Disorders:
Sleep apnea and other sleep disorders disrupt normal sleep by causing breathing problems and frequent awakenings. This poor sleep quality prevents the body from staying in deep sleep. As a result, abnormal sleep behaviors linked to parasomnias are more likely to occur.
4. Medications:
Certain medications increase the risk of parasomnias. Drugs such as antidepressants, antipsychotics, and sedatives affect brain activity during sleep. These changes lead to abnormal behaviors during sleep.
5. Neurological Conditions:
Neurological conditions such as Parkinson's disease, Alzheimer's disease, and dementia affect brain control during sleep. These disorders disrupt normal REM sleep processes. This disruption often leads to parasomnias, especially REM sleep behavior disorder.
6. Genetics:
Parasomnias sometimes run in families, which suggests a genetic link. Inherited traits influence how the brain regulates sleep cycles and arousal. This raises the risk of developing parasomnia behaviors across generations.
7. Substance Use:
Substance use such as alcohol, drugs, and caffeine interferes with normal sleep patterns. These substances disrupt sleep depth and timing. This disruption increases the risk of parasomnias and abnormal sleep behaviors.

Diagnosis of Parasomnias
At Mir Neurology, we employ a comprehensive approach to diagnosing parasomnias, which may involve:
1. Medical History and Symptom Review:
Your doctor will ask you about your sleep patterns, the frequency of symptoms, any associated triggers, and other related health conditions.
It is helpful to keep a sleep diary and note any behaviors or disturbances.
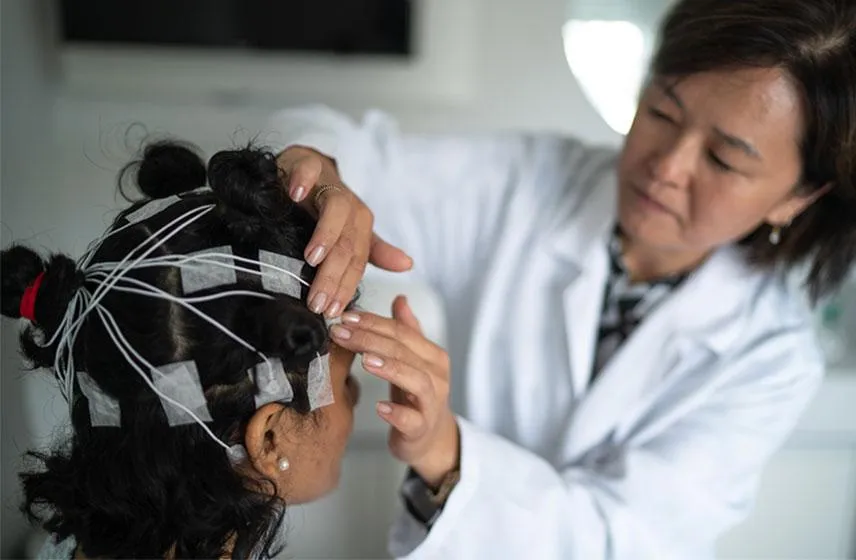
2. Sleep Study (Polysomnography):
A sleep study can be conducted to observe your sleep patterns and identify any abnormal behaviors during sleep.
During the study, sensors will be attached to monitor brain waves, eye movements, heart rate, and muscle activity to better understand the nature of your parasomnias.
3. Actigraphy:
A wrist-worn device tracks sleep and movement patterns over extended periods.
Identifies sleep fragmentation.
Supports long-term treatment planning.
4. Neurological Evaluation:
A detailed exam evaluates nervous system function and underlying conditions.
Identifies early neurological disease
Guides targeted therapy
5. Psychological Evaluation:
Screening and sleep studies help identify the causes of parasomnias. These assessments support accurate diagnosis and improve long-term sleep outcomes.
Screening assesses stress, anxiety, trauma, and mood disorders.
Screening supports integrated treatment planning.
Early assessment improves long-term sleep outcomes.
A sleep study observes sleep patterns and abnormal sleep behaviors.
Sensors monitor brain waves, eye movements, heart rate, and muscle activity.
Findings help identify the type and cause of parasomnias.


Treatment for Parasomnias
Treatment for parasomnias depends on the type of disorder and its severity. Options include:
1. Behavioral Therapy
Cognitive Behavioral Therapy (CBT) is effective for treating parasomnias triggered by stress, anxiety, or trauma. CBT helps individuals change thought patterns and manage emotions that contribute to sleep disturbances.
Sleep Hygiene – Improving sleep habits, maintaining a regular sleep schedule, and creating a relaxing bedtime routine can reduce parasomnia episodes.
2. Medications
In some cases, medications may be prescribed to help control parasomnia symptoms. These may include:
Benzodiazepines (e.g., clonazepam) for sleepwalking or REM Sleep Behavior Disorder.
Antidepressants or melatonin to manage nightmares or sleep-related anxiety.
Anticonvulsants for those with frequent or severe episodes.
3. Safety Measures
For individuals who sleepwalk or have night terrors, making the sleep environment safe by removing obstacles or locking doors can reduce the risk of injury.
Bed rails or other protective measures may be recommended to prevent falls or injury.


4. Treating Underlying Conditions
If parasomnias are linked to other sleep disorders like sleep apnea or neurological conditions, treating those underlying conditions may help alleviate parasomnia symptoms.
Living with Parasomnias
Living with parasomnias requires consistent sleep habits and daily routine management. You should follow a regular sleep schedule to support stable sleep cycles. Stress management helps reduce sleep disruptions during the night. Avoid alcohol, drugs, and excess caffeine before bedtime. A calm bedtime routine supports better sleep quality. Creating a safe sleep environment reduces the risk of injury.
While parasomnias feel disruptive and distressing, proper treatment helps reduce symptoms. At Mir Neurology, you receive support and care focused on improving sleep and overall quality of life.
Get Expert Help

If you or a loved one is experiencing memory loss or cognitive decline, early diagnosis is key to effective management. Consult with our neurology specialists for personalized assessment and care plans.
Our Locations
To learn more about our experience or discuss your treatment options, please call us at (301) 797-7600 or schedule a consultation today!
Get our wellness newsletter
Filter out the noise and nurture your inbox with health and wellness advice that’s inclusive and rooted in medical expertise.
Contact Us
Complaint and Queries
(301) 517-7636
About | Careers
© Copyright 2026. Mir Neurology. All Rights Reserved.
A Part of Highland Healthy Living. Powered By CareSyncMarketing



